PROJECT LEADS: Christine Blauvelt MD, Neda Ghaffari MD, Roxanna Irani MD PhD
EXECUTIVE SPONSOR: Nerys Benfield MD MPH
ABSTRACT: Hypertensive disorders of pregnancy (HDP) are increasingly prevalent, posing significant risks to maternal health, including stroke and renal failure. At UCSF, one quarter of deliveries involve HDP, far exceeding the national average. Postpartum hypertension remains a leading cause of readmission, with about half of postpartum readmissions at UCSF due to hypertension-related issues. This proposal aims to implement a structured remote blood pressure (BP) monitoring program for high-risk patients, utilizing Bluetooth-enabled devices, an integrated APeX dashboard, and nurse-driven protocols for timely intervention. The program aims to improve BP self-monitoring, reduce postpartum length of stay, readmissions and emergency visits, and enhance patient confidence in managing their health. Preliminary data from our pilot program has shown promising results, with enrollees demonstrating high engagement, high patient satisfaction, and a 0% readmission rate for hypertension among postpartum participants. Our pilot has proven the feasibility and clinical importance of this work, and our Caring Wisely proposal aims to further build infrastructure and sustainability into our program so it can ultimately be expanded to all high-risk pregnant and postpartum patients at UCSF.
TEAM:
- Christine Blauvelt, MD (Clinical Fellow, Maternal-Fetal Medicine)
- Roxanna Irani, MD PhD (Associate Professor, Maternal-Fetal Medicine; Ambulatory Executive Director for Women’s Health)
- Neda Ghaffari, MD (Associate Professor, Maternal-Fetal Medicine and Clinical Informatics)
- Martha Tesfalul, MD (Assistant Professor, Maternal-Fetal Medicine)
- Esther Hsiang, MD MBA (Assistant Professor, Department of Medicine; Interim Director of Care Delivery Transformation, Office of Population Health)
- Timothy Judson, MD MPH (Associate Professor, Department of Medicine; Interim Chief Population Health Officer)
- Michael Helle, MBA, MHA (Vice President for Population Health)
- Tasha Toliver (Manager, Office of Population Health)
- Henrietta Tran, MSHE (Manager, Office of Population Health)
- Kristin Gagliardi (Innovation Implementation Specialist, Office of Population Health)
PROBLEM:
Hypertensive disorders of pregnancy (HDP) are increasing in prevalence and pose significant risks to maternal health. These conditions, which include gestational hypertension, preeclampsia, and chronic hypertension with superimposed preeclampsia, can lead to severe complications such as stroke, renal failure, hepatic dysfunction, and cardiovascular disease.1 In 2019 at UCSF, 24.7% of 2,832 delivering patients were diagnosed with a HDP, which is well above the national average of 5-8%.
The definitive management of HDP is delivery of the pregnant person. However, delivery does not always resolve hypertension, and postpartum hypertension (PP HTN) can persist or even worsen in the early postpartum period. Worsening or de novo PP HTN remains the most common reason for acute postpartum evaluation. In 2019, 1.8% of all patients delivering at UCSF were readmitted for PP HTN (data derived from UCSF deidentified clinical data warehouse). The trajectory of postpartum blood pressure (BP) typically peaks between three to six days after delivery, often after hospital discharge. If elevated BP is not promptly addressed in the outpatient setting, it may reach the severe range (over 160/110 mmHg), increasing the risk of stroke due to pregnancy-related physiologic changes and necessitating urgent inpatient evaluation, treatment, and admission.
This unpredictability underscores the importance of empowering patients with knowledge and tools for BP self-monitoring. Previous studies have shown that when patients with HDP monitor their blood pressure at home, there are reduced rates of hypertension-related hospital readmissions and ED visits.2-5 One prospective cohort study of 780 patients demonstrated a reduction of postpartum readmissions or ED visit for hypertension from 11% to 2.8% (aOR 0.24, 95% CI 0.12–0.49, P<.001) with the implementation of a remote blood pressure monitoring program with standardized blood pressure management.2 Another study of 428 women demonstrated fewer hypertension-related readmissions in postpartum patients enrolled in an intervention with telehealth and remote blood pressure monitoring compared with the controls (0.5% vs 3.7%; RR, 0.12; 95% CI, 0.01–0.96).3
Increased confidence in outpatient BP monitoring can have significant institutional and patient-level benefits. Patients who are comfortable with remote BP monitoring are more likely to engage in self-care, recognize concerning symptoms early, and seek appropriate outpatient interventions rather than relying on emergency department visits. At the institutional level, reducing unnecessary postpartum evaluations and admissions alleviates provider burden, enhances resource allocation, and improves overall patient satisfaction. The ability to safely discharge patients with an effective outpatient monitoring system may also contribute to a reduced postpartum length of stay without compromising patient safety.
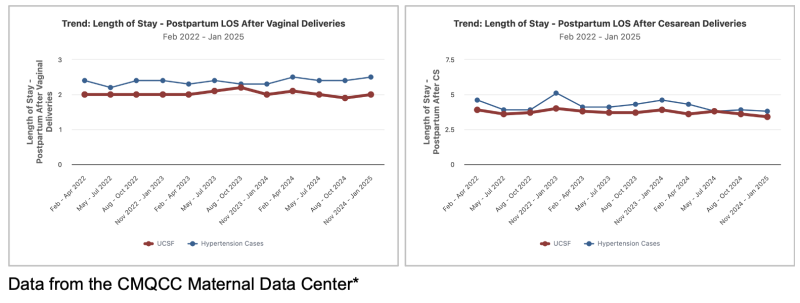
Patients with HDP consistently have longer postpartum LOS than those without, likely driven by inpatient blood pressure monitoring and medication titration (Figure 1: Postpartum LOS at UCSF by Hypertension Status). Our labor and delivery unit has historically required 24 hours of observation after any medication dose adjustment. In February 2024, this protocol was revised to 6-12 hours of observation after dose adjustments, yet provider hesitation remains regarding same-day discharge after medication changes. A structured remote BP monitoring program could increase provider confidence in earlier discharge while ensuring patient safety. Over time, broader adoption of remote BP monitoring will help align inpatient protocols with these evolving care models.
In 2023, the UCSF Division of Maternal-Fetal Medicine partnered with the Office of Population Health to launch a remote BP monitoring pilot program for peripartum patients with or at high risk of developing HDP. The program infrastructure included an APeX-integrated hypertension dashboard that consolidates data from Bluetooth-enabled BP devices (Figure 2: APeX BP Display), clinical decision-support including medication titration and escalation pathways, and a centralized team to engage with and monitor patients. The goal of the program was to demonstrate proof of concept and establish feasibility for a remote monitoring program to improve BP control for peripartum patients.
The pilot has enrolled 55 patients with or at high risk of developing a HDP. The pilot program demonstrated strong engagement with remote monitoring: 94% remotely transmitted at least one BP per week 75% of the time, and 88% had a BP measurement within 10 days of delivery (ACOG best practice recommendation1). Pilot participants had a shorter postpartum length of stay (LOS) compared to historical UCSF data (Pilot: 2.7 days overall, 2.5 days for those enrolled prior to delivery; Historical: 3.0 days for patients with HDP). Qualitative interviews highlighted high patient satisfaction, with participants valuing the ease of a technology-enabled solution, the support from the nurse monitoring team, and the structure it provided in developing consistent BP monitoring and medication adherence habits. Additionally, postpartum enrollees had a 0% readmission rate for hypertension compared to 5% among non-participants. This preliminary data suggests several potential benefits of remote BP monitoring for high-risk patients, warranting further investigation and expansion of the program.
TARGET:
By June 2026, we will expand the remote BP monitoring program to 100 additional participants who are at high-risk of HDP at UCSF. Our clinical goals are to increase patient engagement in BP self-monitoring, reduce postpartum length of stay, reduce postpartum readmissions and OB ED visits for HTN, and improve patient confidence in at-home BP management. Our program goals are to build sustainability and efficiency into the remote BP monitoring system so it can be expanded to all high-risk patients at UCSF.
Target Quantitative Outcomes:
- ≥95% of enrolled patients will report weekly BP at least 75% of the time
- ≥95% of postpartum participants will have a BP measurement within 10 days of delivery.
- 0.5 day reduction in postpartum length of stay for patients with HDP
- 50% reduction in postpartum readmissions for HTN-related complications
- 50% reduction in OB ED visits for HTN-related complications to improve healthcare quality and patient experience.
Target Qualitative Outcomes:
- Improved patient confidence in self-monitoring and managing BP, as assessed through post-program surveys and qualitative interviews.
- Enhanced provider efficiency through automated risk stratification and streamlined nurse-led interventions, reducing unnecessary emergency visits.
- Greater health equity by ensuring access to BP monitoring tools and education for patients from diverse backgrounds, addressing potential barriers related to language, digital literacy, and socioeconomic status.
GAPS:
Several systemic, technological, and education gaps have historically contributed to poor outpatient BP control and delayed interventions, leading to HDP-related morbidity and costs.
System Issues:
- Lack of standardized postpartum BP monitoring protocols: Many patients are discharged with minimal guidance on BP self-monitoring and follow-up care.
- Limited care coordination: Patients often experience fragmented care due to unclear pathways for outpatient BP management and difficulty accessing timely follow-up appointments.
- Health disparities and inequities: Social determinants of health, such as limited access to medical devices, transportation barriers, and digital literacy challenges, disproportionately affect marginalized populations.
Technological Gaps:
- Limited integration of home BP monitoring into the EHR: Existing systems do not allow for seamless tracking of BP trends, limiting real-time provider intervention.
- Inefficient alert systems: Current workflows do not prioritize automated notifications for high-risk BP elevations, delaying clinical action.
Educational Gaps:
- Patient knowledge gaps: Many individuals do not fully understand the risks of hypertensive disorders of pregnancy or how to manage it at home.
- Low patient confidence in self-management: Many postpartum individuals report anxiety about at-home BP monitoring, leading to decreased adherence and increased emergency department utilization.
INTERVENTION:
We propose a remote BP monitoring program leveraging Bluetooth-enabled devices, an EHR-integrated dashboard, and standardized nurse-driven protocols (Figure 3: Program Workflow).
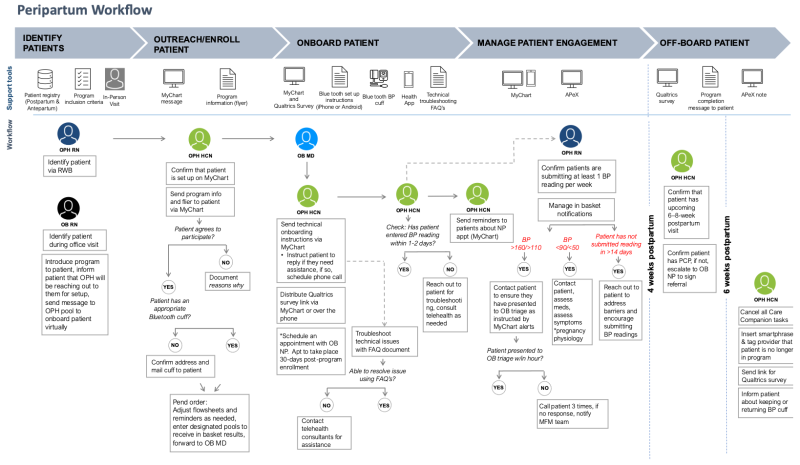
Technology-Enabled Remote BP Monitoring: High-risk patients will receive Bluetooth-enabled blood pressure monitors to facilitate remote tracking and improve hypertension management. An APeX-integrated dashboard displays real-time BP data, allowing clinical teams to efficiently monitor trends and identify patients requiring intervention. Additionally, an automated alert system flags severe BP elevations, enabling timely provider response and reducing delays in care.
Healthcare Navigator and Nurse-Driven Telehealth Support: Eligible patients will be contacted and enrolled by healthcare navigators, who will also assist with BP device set-up. Patients will have regular virtual check-ins with nurses trained in hypertension management to ensure ongoing support and adherence to treatment plans. Standardized protocols will guide BP management, including medication titration and care escalation based on real-time data. Direct communication pathways between nurses and obstetric providers will facilitate rapid intervention, improving patient outcomes and reducing the risk of complications.
Patient Education and Engagement: Patients will receive education on BP self-monitoring, medication adherence, and symptom recognition to enhance their confidence in managing hypertension. MyChart reminders will reinforce adherence to BP monitoring and follow-up visits, ensuring consistent engagement. Early antepartum education will introduce self-monitoring before delivery, helping patients become comfortable with the process and improving postpartum adherence.
Equity: We plan to continue a focus on populations with known health disparities in peripartum health. We will reserve at least 10% of program spots for eligible Black/African-American patients, who experience disproportionately high rates of HDP and related complications. We will continue to recruit from our Black concordant care programs for pregnant patients (Black Wellness Clinic). Multilingual support has been integrated into educational materials and telehealth visits to accommodate diverse patient populations. Digital literacy assistance will be available through one-on-one support for patients unfamiliar with technology, helping them navigate remote monitoring tools. Additionally, a tailored outreach system will proactively engage diverse patient populations, including by race/ethnicity and insurance status. This initiative aligns with UCSF’s commitment to reducing maternal health disparities and improving postpartum outcomes through innovative, patient-centered, and technology-driven care models.
PROPOSED EHR MODIFICATIONS:
Currently, we use an APeX-integrated BP monitoring dashboard that displays BP readings from Bluetooth-enabled devices and generates automated alerts for severe BP elevations. However, enhancements to our APeX integration could allow for more informed decision-making and make the program more efficient and sustainable.
- Enhanced BP Monitoring Display: To support scalability and streamline clinical decision-making, we will expand the APeX hypertension dashboard to consolidate key clinical data. Proposed additions include HDP diagnosis, current medications, gestational age or weeks postpartum, and a flowsheet containing BP readings, medication adjustments, and OB ED visits/admissions (Figure 4: Hypertension Dashboard).
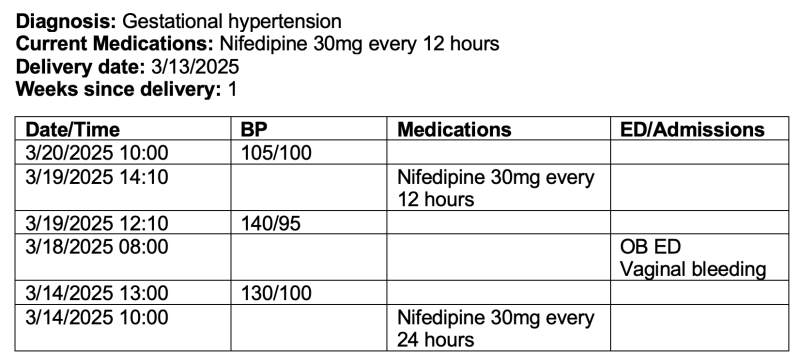

- Standardized Outpatient Order Set Addendums: Develop structured order sets to guide outpatient BP management, including recommended medication titrations based on severity.
- Automated Patient Alerts for Severe Hypertension: We propose implementing an automated patient alert system to immediately notify patients when they record a dangerous BP, prompting them to seek urgent medical attention. While our care team will continue to receive alerts and conduct patient outreach, this automated system will provide an additional layer of safety within the remote BP monitoring program.
RETURN ON INVESTMENT (ROI):
Reduce postpartum hospital stay by 0.5 days
Metric | Calculation |
Direct cost of 1 day postpartum LOS | $3841.82 |
Projected reduction in postpartum LOS | 100 participants * 0.5 day reduction = 50 days |
Projected cost savings | 50 days * $3841.81/day = $192,091 |
Reduce PP HTN readmissions by 50%
Metric | Calculation |
Number of PP HTN readmissions/year | 7% * 100 participants = 7 readmissions |
Total days of reduced PP readmissions | 7 readmissions * 50% * 2 days = 7 days |
Backfill volume of new incremental admissions | 7 days / 4 day LOS = 1.75 admissions |
Projected additional revenue from new incremental admissions | 1.75 admissions * $7500 = $13,125 |
Increased provider capacity
Automated BP risk stratification and streamlined nurse-led interventions will reduce the need for obstetric providers to follow-up these patients, allowing them to see a higher volume of other patients.
Our nursing team currently spends approximately 0.17 hours per patient per week on BP review and management. When individual clinicians perform this task, we estimate their efficiency is lower than our nursing team, as they lack the streamlined systems developed by our team. Therefore, we estimate that clinicians would require 0.2 hours per patient per week, equating to 0.4 CPT level 3 follow-up visits per patient per week.
The projected revenue from additional visits ($165/visit) is based on UCSF reimbursement data from 2023, weighted according to the observed payor mix in the pilot.
Metric | Calculation |
Additional provider visits per patient per week | 0.4 visits |
Average duration of program involvement per patient | 12 weeks |
Reimbursement from additional visit (CPT level 3 f/u) | $165 |
Projected additional revenue from new incremental visits | $165 * 0.4 visits * 12 weeks * 100 patients = $79,200 |
TOTAL COST SAVINGS / ADDITIONAL REVENUE: $284,416/year
SUSTAINABILITY:
As part of ensuring sustainability of the program, we have assembled a large team consisting of inpatient and outpatient providers and staff, as well as key leaders in the department. This team monitors outcomes at monthly and quarterly intervals and revisits protocols to improve and maintain the program. We also plan to build APeX modifications that will make the program more efficient and allow us to support future program expansion. Additionally, we are exploring reimbursement modalities for remote patient monitoring and other additional funding avenues to offset some of the costs required to sustain the program (i.e. equipment replacement). Finally, participants will be asked to return their BP device at postpartum visits and/or will be provided materials to mail the BP devices back, which will allow them to be used by other participants.
BUDGET:
Item | Cost |
Bluetooth enabled BP cuff ($77) Assumes 50% equipment return rate | $77 * 100 patients * 50% = $3850 |
Nursing support 1.0 FTE covers 960 patients | 0.10 FTE * $282,000 = $28,200 |
Healthcare navigator support 1.0 FTE covers 1000 patients | 0.10 FTE * $126,000 = $12,600 |
APeX modifications Consultant time | $100/hr * 53.5 hours = $5350 |
TOTAL | $50,000 |
REFERENCES:
- American College of Obstetricians and Gynecologists. "Gestational hypertension and preeclampsia: ACOG practice bulletin, number 222." Obstet Gynecol 135.6 (2020): e237-e260.
- Mei JY, Corry-Saavedra K, Nguyen TA, Murphy AM. A standardized clinical assessment and management plan (SCAMP) reduces readmissions in postpartum hypertension. American Journal of Obstetrics & Gynecology. 2023;228(1):S18-S19.
- Hoppe KK, Williams M, Thomas N, et al. Telehealth with remote blood pressure monitoring for postpartum hypertension: a prospective single-cohort feasibility study. Pregnancy hypertension. 2019;15:171-176.
- Hauspurg A, Lemon LS, Quinn BA, et al. A postpartum remote hypertension monitoring protocol implemented at the hospital level. Obstetrics and gynecology. 2019;134(4):685.
- Suresh SC, Duncan C, Kaur H, et al. Postpartum outcomes with systematic treatment and management of postpartum hypertension. Obstetrics & Gynecology. 2021;138(5):777-787.

Comments
We've observed excellent
We've observed excellent results in our initial pilot of HTN monitoring for OB patients. There's a real opportunity to build on this work to create sustainable workflows and expand this to more patients in need, decreasing unnecessary ED visits and hospitalizations, particularly for vulnerable populations. Dr. Blauvelt's proposal has my full support.
Congratulations on a
Congratulations on a successful pilot! A few more questions would help to clarify your submission:
1. Now that you have completed 1 PDSA of your program, can you identify implementation GAPs that need to be addressed in order to improve its adoption and effectiveness? How do the proposed EHR modifications address implementation gaps that you've measured or observed in your pilot?
2. How did you arrive at a 1 day reduction in ALOS? Studies cited show consistent impact of these programs on readmission rates. Are there studies that show reduction in hospital LOS?
3. Sustainability. As you are using a significant amount of funding to pay for care delivery staffing of the program, can you provide more concrete commitment from health systems operations leaders that will ensure funding for these positions after Caring Wisely funding ends?
Thank you for your thoughtful
Thank you for your thoughtful questions, Dr. Gonzales! We apologize for the delay in our response as we gathered additional data to provide the most comprehensive answers.
1) Our initial PDSA cycle identified several implementation gaps, some of which we have already addressed in preparation for the second cycle. For cycle 2, we aim to address additional gaps, with EHR modifications playing a critical role in improving program efficiency and patient safety.
Gaps Addressed in Cycle 1:
Gaps to Address in Cycle 2:
2) Thank you for raising this important point. We have revised our proposal from a 1-day to a 0.5-day reduction in postpartum LOS based on review of historical UCSF data and data from our pilot program. For this analysis, we defined postpartum LOS as the time between delivery and hospital discharge. At UCSF, patients with HDP have an approximately 0.5-day longer postpartum LOS than those without HDP. Patients on antihypertensive medications have even longer postpartum hospitalizations (average postpartum LOS of 3.4 days in 2023).
Prolonged LOS in patients with HDP is primarily driven by inpatient blood pressure monitoring and medication titration, historically requiring 24 hours of observation after any medication dose adjustment. In February 2024, this protocol was revised to 6-12 hours of observation after dose adjustments, yet provider hesitation remains regarding same-day discharge after medication changes. A structured remote BP monitoring program could increase provider confidence in earlier discharge while ensuring patient safety. Over time, broader adoption of remote BP monitoring will help align inpatient protocols with these evolving care models.
Postpartum Length of Stay at UCSF
Fiscal Year
HDP
Non-HDP
FY23
2.9
2.5
FY24
3.1
2.6
FY25 (until 11/9/2024)
3.0
2.5
Our pilot data suggests that a reduction in postpartum LOS is feasible. Participants in our pilot program had an average postpartum LOS of 2.7 days, approximately 0.3 days shorter than the overall HDP population at UCSF. Pilot participants who were enrolled prior to delivery had an even shorter postpartum LOS of 2.5 days. We acknowledge that few published studies specifically demonstrate a reduction in postpartum LOS with remote BP monitoring, with most focusing on readmission rates and other post-discharge metrics (such as recorded BP within 7-10 days) as their primary outcome. Those that do report postpartum LOS often report this metric in days rather than hours, potentially overlooking small but meaningful reductions in LOS that impact hospital costs, staffing, and bed availability.
We also generated more precise cost-savings projections using service-line budget reports from 2024 and 2025 obstetric delivery hospitalizations. The direct costs of a delivery hospitalization include several fixed costs associated with the delivery itself. To estimate cost savings from reducing postpartum length of stay, we focused on the direct costs of the last full day of admission, as this more accurately reflects postpartum hospitalization costs. In 2024–2025, the average direct cost for the last full day of admission was $3841.82.
Metric
Calculation
Direct cost of 1 day postpartum LOS
$3841.82
Projected reduction in postpartum LOS
100 participants * 0.5 day reduction = 50 days
Projected cost savings
50 days * $3841.81/day = $192,091
3) We agree that long-term sustainability of this program will require formal commitment from health systems operations leaders beyond the Caring Wisely funding period. We are actively working with UCSF’s Office of Population Health to submit a formal proposal to health system leadership for ongoing funding of key program staff and other resources.
Expanding our pilot through the Caring Wisely program will generate additional data on clinical impact and cost savings, while strengthening program infrastructure for greater efficiency and sustainability. This will help us secure funding from health systems operations leaders for widespread and long-term adoption of a remote BP monitoring program for pregnant patients at UCSF.
Great project! Very excited
Great project! Very excited to see this come to fruition. Hospital overcrowding is one of the biggest challenges we're facing and upstream efforts to reduce hospitalization are crucial.
Thank you so much for your
Thank you so much for your support of our work!
Thanks for your submission of
Thanks for your submission of this excellent proposal. A few comments/questions:
1) Are the gaps that are listed in the proposal gaps that currently exist even after the pilot, or are they gaps that existed at the start of the project. If the latter, what are the current, ongoing gaps beyond availability of more bluetooth enabled BP cuffs to enroll more patients and human resources to enact the pathway?
2) For the projected revenue due to providers having more time to see patients instead of managing peripartum and postpartum hypertension, is the time saved per patient based off of timestudy data from the pilot or is a guesstimate from providers?
3) Have you consulted with UCSF Health informatics to see if the proposed EHR enhancements are feasible and doable within a Caring Wisely project year?
4) I agree with Ralph's comment above that I would like more information on where the 1 day LOS reduction (which is a lot!) projection is predicted on. Information in the medical literature? I didn't see any LOS reduction reported in the pilot.
Thank you so much for these
Thank you so much for these questions and feedback on our proposal!
1) The gaps listed in our proposal reflect those that existed at the start of the project, many of which we have successfully addressed through our pilot. We developed standardized BP monitoring protocols for both patients and providers, including educational handouts outlining BP thresholds requiring clinical attention and key symptoms of HDP, as well as protocols for medication adjustments. We also improved care coordination for patients with HDP. Our use of Bluetooth-enabled BP cuffs with APeX integration enables real-time BP monitoring by our nursing team. In contrast, patients not enrolled in the remote BP monitoring system rely on scheduled visits to review BP readings—these appointments are limited and often delayed, increasing the risk of missed intervention.
In the next phase, we aim to enhance efficiency and patient safety by expanding the APeX Hypertension Dashboard and implementing automated patient alerts for severe hypertension. The enhanced dashboard will consolidate key clinical data, including HDP diagnosis, medications, gestational age/postpartum weeks, and a BP flowsheet, supporting streamlined patient management. Additionally, we propose an automated alert system to notify patients of dangerously high BP readings, prompting urgent medical attention while maintaining provider oversight. These improvements will help scale the program to all high-risk patients at UCSF.
2) The original projected revenue was based on a rough estimate from providers on the time spent reviewing patients’ BP logs and contacting them to discuss clinical management. However, we have now refined this estimate with a more precise calculation:
Our nursing team currently spends approximately 0.17 hours per patient per week on BP review and management. When individual clinicians perform this task, we estimate their efficiency is lower than our nursing team, as they lack the streamlined systems developed by our team. Therefore, we estimate that clinicians would require 0.2 hours per patient per week, equating to 0.4 CPT level 3 follow-up visits per patient per week.
For cost estimation, we used a more conservative reimbursement rate of $165 for a CPT level 3 follow-up visit (based on UCSF reimbursement data from 2023, weighted according to the observed payor mix in the pilot).
Metric
Calculation
Additional provider visits per patient per week
0.4 visits
Average duration of program involvement per patient
12 weeks
Reimbursement from additional visit (CPT level 3 f/u)
$165
Projected additional revenue from new incremental visits
$165 * 0.4 visits * 12 weeks * 100 patients = $79,200
We recognize that when clinicians perform BP reviews, they may not have the bandwidth to review data in as much detail as our dedicated nursing team. If clinicians spent only 0.1 hours per patient per week, revenue from additional visits would decrease, but this would also result in tradeoffs in quality of BP data review and management.
3) We worked with UCSF IT to build the APeX integration and dashboard for the pilot. We are currently collaborating with Marty Schroeder to assess the feasibility of the proposed EHR changes, and we will update you as we gather more information.
4) Thank you for this comment! We hope we have addressed your question in our response to Dr. Gonzales. We have revised our proposal to a more conservative 0.5-day reduction in postpartum LOS based on historical data from UCSF and data from our pilot program. Participants in our pilot had a 2.7-day postpartum LOS and those enrolled prior to delivery had a 2.5-day postpartum LOS, which was shorter than historical data (HDP: 3.0 days; HDP on medications: 3.4 days).